Recognizing the Signs of Persistent Depressive Disorder: A Research-Based Guide for 2026

Did you know that approximately 1.5% of adults in the United States live with a low-grade, heavy fog that doesn't lift for years at a time? Many people I meet in my practice have spent over 730 consecutive days feeling perpetually gloomy or low on energy, often assuming it's just a permanent part of their personality. If you've felt functional but unfulfilled for a long period, you aren't just experiencing a run of bad luck. You may be experiencing the specific signs of persistent depressive disorder, a chronic condition that requires a distinct, clinical approach to resolve.
It's common to feel confused when your experience doesn't match the acute, crashing nature often associated with major depression. I understand the weight of living in this middle ground where you're getting by but not truly thriving. This guide provides you with clinical clarity on your symptoms and offers an evidence-based roadmap to recovery based on 2026 research. We'll examine the physiological markers of this condition and the structured, data-driven steps you can take to move toward a more vibrant, clear-headed life.
Key Takeaways
- Understand the "two-year rule" and how clinical duration serves as the primary differentiator for a formal Persistent Depressive Disorder diagnosis.
- Learn to recognize the subtle behavioral and cognitive signs of persistent depressive disorder, including how chronic low-grade symptoms disrupt executive functioning.
- Gain clarity on the critical differences between PDD and Major Depressive Disorder, focusing on the "waxing and waning" nature of long-term mood patterns.
- Discover the vital role of a board-certified psychologist in moving beyond self-diagnosis to create a precise, evidence-based roadmap for your recovery.
- Explore how targeted interventions like CBT and ACT provide a scientific path forward by challenging chronic negative thought patterns and restoring your quality of life.
Defining Persistent Depressive Disorder: Beyond the Two-Year Mark
Persistent Depressive Disorder (PDD) represents a chronic form of depression that often flies under the clinical radar because of its low-intensity, long-term nature. According to the DSM-5-TR, the primary diagnostic requirement is the "Two-Year Rule." For an adult to receive this diagnosis, they must experience a depressed mood for most of the day, for more days than not, for at least two years. In children and adolescents, this duration requirement is reduced to one year. This temporal benchmark is what separates PDD from Major Depressive Disorder (MDD), which typically presents in shorter, more severe episodes.
The medical community previously categorized this condition as Dysthymia (Persistent Depressive Disorder). In modern practice, PDD now serves as an umbrella term that includes both the old definition of dysthymia and chronic major depressive episodes. Research from the National Institute of Mental Health indicates that PDD affects approximately 1.5% of U.S. adults every year. Despite this, it's common for individuals to live with these symptoms for 10 to 30 years before seeking help. They don't realize their experience is a treatable clinical condition; they simply assume it's who they are.
The Myth of the Gloomy Personality
I frequently meet patients who describe themselves as "naturally cynical" or "just a serious person." It's vital to distinguish between an introverted temperament and clinical PDD. While a temperament is a stable part of your personality, PDD is a persistent weight that dampens your ability to feel joy or maintain energy. Over time, this chronic low mood becomes a "new normal," masking the underlying signs of persistent depressive disorder as mere personality traits. Persistent Depressive Disorder is a physiological and psychological state, not a character flaw.
Double Depression: When PDD and MDD Co-occur
The clinical landscape becomes more complex when a person with PDD experiences a "spike" in symptoms that meets the criteria for a major depressive episode. This phenomenon is known as "Double Depression." In these cases, the individual lives at a baseline of mild sadness or fatigue, but then falls into a much deeper, more acute period of despair. These cycles can be incredibly draining, as the person never truly returns to a state of high functioning or wellness between episodes.
Recognizing these overlapping patterns is a primary goal of the diagnostic process. I focus on uncovering the "why" behind these shifts to provide you with a clearer roadmap for recovery. Gaining this level of insight starts with a thorough psychological assessment near me. By identifying the specific signs of persistent depressive disorder versus acute MDD, we can create a precise strategy to improve your daily quality of life and restore a sense of stability.
The Primary Behavioral and Cognitive Signs of Persistent Depressive Disorder
Identifying the signs of persistent depressive disorder (PDD) requires a nuanced eye because the symptoms don't always scream for attention. Instead, they whisper. Unlike the acute, crashing sensation often associated with major depression, PDD is defined by its pervasive, low-grade nature. For a diagnosis in adults, these symptoms must be present for at least two years. I often describe it to my patients as a low-level static that interferes with the clarity of daily life, making the world feel perpetually gray rather than black and white.
Executive functioning is one of the first areas to erode under the weight of chronic depression. This manifests as a persistent difficulty in making decisions, even minor ones like choosing a lunch order or a driving route. Concentration often feels like wading through a thick fog. According to NIMH statistics on Persistent Depressive Disorder, this condition affects approximately 1.5% of U.S. adults annually, with many individuals struggling for years before seeking a formal evaluation.
Physical manifestations are equally telling. Chronic fatigue is a hallmark, but it's rarely cured by a full night's sleep. Instead, patients report "non-restorative" sleep, where they wake up feeling just as depleted as when they went to bed. Appetite changes may be gradual, such as a slow weight gain or loss of 5% of body mass over several months. Socially, PDD leads to a subtle withdrawal. It's not a sudden isolation, but rather a slow decline in social engagement. You might find yourself saying "no" to invitations for 18 months straight because the emotional energy required for interaction feels too high.
Emotional and Self-Perceptual Symptoms
Low self-esteem serves as the bedrock of this disorder. It's a pervasive self-criticism that colors every achievement and interaction. When I work with patients, I see how hopelessness acts as a quiet, steady belief that things won't truly improve. This isn't a loud despair; it's a resigned acceptance. PDD distorts the perception of time. The past is viewed as a series of missed opportunities, the present feels like an exhausting chore, and the future is seen as more of the same. This cognitive "filter" makes it difficult to remember a time when things felt genuinely light or joyful.
Functional Impairment in Daily Life
Many individuals with PDD fall into the category of "high-functioning" depression. They maintain their careers, pay their bills, and fulfill family obligations, but the hidden cost is immense. Over a 5-year or 10-year period, the strain of "masking" symptoms leads to significant burnout and relationship instability. The effort required to appear productive leaves no energy for genuine connection. Functional capacity does not negate the need for clinical intervention. If you feel like you're merely surviving your schedule, gaining clarity through a neuropsychological roadmap can help you move toward a more vibrant, engaged life.
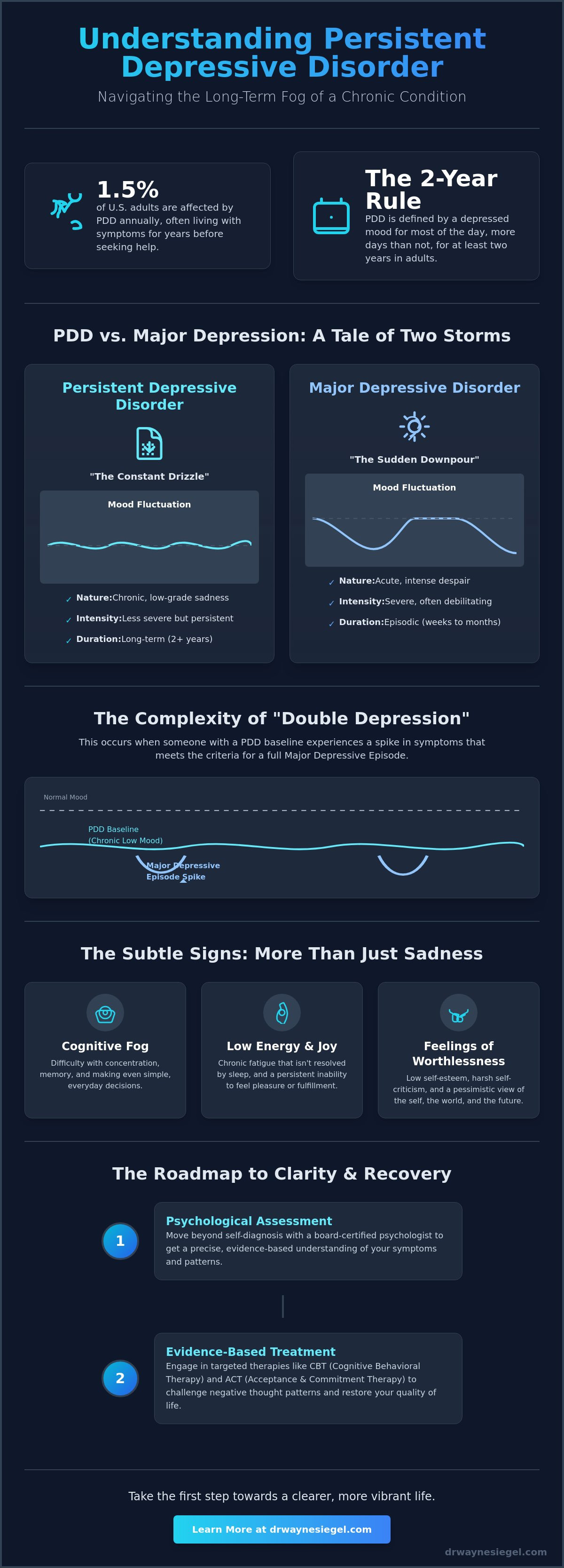
PDD vs. Major Depressive Disorder: Key Differences
Distinguishing between Persistent Depressive Disorder (PDD) and Major Depressive Disorder (MDD) is a critical step in creating an effective roadmap for recovery. While they share common emotional ground, their clinical profiles differ significantly in terms of temporal patterns and symptom intensity. MDD is typically characterized by acute episodes that represent a sharp departure from a person's previous level of functioning. In contrast, PDD is defined by its endurance. In my practice, I find that patients with PDD don't describe a sudden storm; instead, they describe a persistent fog that has become part of their daily landscape.
Research from the Mayo Clinic highlights that the signs of persistent depressive disorder often include a low mood that lasts for at least two years in adults. During this 730-day period, symptoms may wax and wane, but they never fully disappear for more than two months at a time. This differs from MDD, where symptoms must be present for at least 14 days and are usually more severe, often involving significant disruptions to sleep, appetite, and physical energy. Understanding these signs of persistent depressive disorder helps us move beyond temporary fixes toward a sustainable solution.
Diagnostic Criteria Breakdown
The DSM-5 provides a clear framework for this distinction. To meet the criteria for PDD, an adult must experience a depressed mood for most of the day, for more days than not, for at least two years. In children and adolescents, this requirement is shortened to one year. I often look at the age of onset to gain deeper insight into the patient's journey. Early-onset PDD occurs before age 21 and is frequently linked to a higher likelihood of comorbid personality disorders. Late-onset PDD occurs at age 21 or older. Common diagnostic markers include:
- Feelings of hopelessness that persist for years.
- Low self-esteem that feels like a permanent personality trait.
- Chronic fatigue that doesn't resolve with rest.
- Difficulty making decisions or concentrating on complex tasks.
The Burden of Chronicity
While MDD symptoms are often more intense, the cumulative effect of PDD is equally disabling. Living with a constant, low-level sadness for years erodes a person's sense of self and their belief that life can be different. This psychological toll is heavy; it leads to a state where the individual never feels fully well or energetic. Without intervention, PDD can evolve into "double depression," where a major depressive episode is superimposed on the chronic low mood. Gaining clarity on these patterns is essential. This is why choosing a clinic for psychology that prioritizes evidence-based, long-term therapeutic strategies is a vital part of your journey toward wellness.
The Roadmap to Clarity: Evidence-Based Psychological Assessment
Identifying the signs of persistent depressive disorder requires a level of precision that a standard online checklist cannot provide. Because PDD symptoms must persist for at least two years, they often weave themselves into the fabric of your identity. You might feel like your low mood is simply "who you are" rather than a clinical condition that responds to treatment. I've observed that self-diagnosis frequently leads to confusion between chronic depression and other personality-based struggles. A board-certified psychologist provides the objective lens necessary to separate your personality from your pathology.
In my practice, I view the diagnostic process as the first step toward relief. We don't just look for a label; we look for the "why" behind your experience. By 2026, psychological science has advanced to allow for more nuanced profiling. We use these tools to ensure that your treatment plan is built on a foundation of data rather than guesswork. This clarity is essential for moving from a state of quiet endurance to one of active recovery.
The Assessment Process
The clinical interview is the cornerstone of our work together. We carefully map your emotional history over the past 24 months to understand the frequency and intensity of your symptoms. Following this, I utilize standardized psychological testing, such as the MMPI-3, which compares your responses against a normative database of thousands of individuals. This helps us measure the specific cognitive impact of your mood. We also perform critical "rule-outs." Research indicates that approximately 10% of depressive symptoms are actually rooted in medical issues like thyroid dysfunction or neurodivergent traits like ADHD. We leave no stone unturned to ensure your diagnosis is accurate.
Moving Beyond the Label
A formal assessment does more than name your struggle; it uncovers your cognitive and emotional assets. I focus on identifying your unique strengths, such as your intellectual resilience or your capacity for insight, which we'll use as levers in your treatment. We shift the narrative from "having a problem" to "having a plan." This transition is empowering because it replaces vague distress with a concrete, actionable roadmap. This assessment serves as a collaborative partnership where we work together to decode your experiences and build a sustainable path forward.
If you're ready to gain a clearer understanding of your mental health, I invite you to learn more about how a professional neuropsychological evaluation can provide the answers you need.
Evidence-Based Treatment: CBT, ACT, and the Path Forward
Persistent Depressive Disorder (PDD) is often described as a marathon rather than a sprint. Because the signs of persistent depressive disorder typically endure for two years or more, the brain develops deeply ingrained neural pathways associated with low mood and self-criticism. Research published in The Lancet suggests that for chronic cases, a combination of psychotherapy and medication often produces superior results compared to either treatment alone. I've found that a structured, evidence-based approach provides the clarity needed to break these long-standing cycles.
Therapeutic Approaches for Chronic Depression
Cognitive Behavioral Therapy (CBT) remains a gold standard for addressing the "gloomy" cognitive bias inherent in PDD. This bias acts as a mental filter, automatically dismissing positive events while magnifying perceived failures. We use CBT to identify these automatic thoughts and replace them with more balanced, evidence-based perspectives. This process doesn't just change how you think; it changes how your brain processes daily stressors.
Acceptance and Commitment Therapy (ACT) offers a different, complementary strategy. Rather than fighting against every difficult emotion, ACT focuses on psychological flexibility. You learn to observe your symptoms without letting them dictate your actions. This allows you to re-engage with your core values, such as family, career, or personal growth, even on days when your energy is low. For many, PDD is intertwined with past experiences. If trauma is a factor, incorporating specific ptsd counseling techniques can help resolve the underlying nervous system dysregulation that fuels chronic low mood.
Starting Your Journey to Wellness
The landscape of mental health care is more accessible in 2026 than ever before. The expansion of psypact states means that patients can now access specialized neuropsychological care across state lines. This is particularly beneficial for those seeking a clinician who understands the nuances of the signs of persistent depressive disorder and its impact on executive functioning. Telehealth removes the logistical barriers of travel, making it easier to maintain the consistency required for long-term recovery.
Taking the first step involves a professional consultation to establish a clear diagnostic profile. We look beyond the symptoms to understand your unique cognitive strengths and challenges. PDD is a heavy burden to carry, but it's treatable. With the right roadmap and a commitment to evidence-based interventions, achieving remission and a higher quality of life is a realistic, attainable goal. You don't have to navigate this landscape alone. Clarity is possible, and your journey toward a lighter, more purposeful life can begin today.
Moving Toward Clarity and Lasting Change
Navigating a chronic low mood requires more than just endurance; it demands a precise, evidence-based roadmap. Identifying the signs of persistent depressive disorder is a critical milestone in your journey toward wellness. Research from the DSM-5-TR confirms that this condition persists for at least two years, often blending into one's sense of self. My goal is to help you untangle these symptoms through a rigorous psychological assessment. With over 25 years of experience as a board-certified clinical psychologist, I've seen how personalized clarity transforms lives. We'll use proven methodologies like CBT and ACT to shift from surviving to thriving. Through PsyPact telehealth services, I provide this high level of care to patients across the country. You're not defined by your diagnosis. You deserve a partner who values both scientific precision and your unique human experience.
Schedule a consultation with Dr. Wayne Siegel to gain clarity on your mental health journey.
It's time to start your next chapter with the support and expertise you need.
Frequently Asked Questions
Can you have persistent depressive disorder and still be successful?
Yes, you can maintain a high level of professional success while living with this condition. Many individuals I see in my practice are "high-functioning," meaning they meet work deadlines and social obligations despite a constant low mood. Research published in the Journal of Affective Disorders in 2023 indicates that PDD affects 3% of the U.S. population. While you might achieve your goals, the internal effort required often leads to profound exhaustion or burnout over time.
How is persistent depressive disorder different from just being sad?
The primary distinction lies in the duration and consistency of the symptoms. While sadness is a transient emotional response to specific events, PDD involves a depressed mood that lasts for at least two years in adults. According to the DSM-5-TR, this low mood must be present for most of the day on more days than not. It's a chronic state rather than a temporary reaction; it often alters your baseline personality and cognitive profile over several years.
Is persistent depressive disorder permanent, or can it be cured?
PDD is a chronic condition, but it's not a permanent sentence without hope for relief. Clinical studies show that a combination of psychotherapy and medication leads to significant symptom reduction in approximately 60% of patients. I focus on creating a roadmap for recovery that emphasizes long-term management. While the word "cure" is rarely used in clinical psychology, achieving a state of remission where symptoms no longer interfere with daily life is a realistic and measurable goal.
What are the most common early warning signs of PDD?
The early signs of persistent depressive disorder often manifest as subtle shifts in your energy levels and self-perception. You might notice a consistent lack of appetite or overeating, coupled with insomnia or sleeping too much for several weeks. Other indicators include low self-esteem and difficulty making decisions. These symptoms often develop slowly, making them hard to identify until they've persisted for months. I look for these patterns during a neuropsychological assessment to ensure an accurate diagnosis.
Can children or teenagers be diagnosed with persistent depressive disorder?
Yes, children and adolescents can receive a PDD diagnosis, though the clinical criteria differ slightly from adults. For younger patients, the depressed or irritable mood only needs to persist for one year instead of two. Data from the CDC shows that 3.2% of children aged 3 to 17 have been diagnosed with depression. In my practice, I often see this manifest as irritability or declining school performance rather than the typical sadness seen in adults.
Does PDD require medication, or is therapy enough?
Treatment plans are highly individualized, but research suggests that a combined approach is often the most effective. A 2020 meta-analysis in World Psychiatry found that combining Cognitive Behavioral Therapy (CBT) with medication outperformed either treatment alone for chronic depression. Therapy provides the tools for cognitive restructuring, while medication can help stabilize the underlying biological components. My goal is to help you find the specific balance that provides the most clarity and functional improvement for your life.
How do I know if I should see a psychologist for my low mood?
You should consider a consultation if your low mood persists for more than two consecutive weeks or starts to impact your daily functioning. If you find yourself withdrawing from social activities or struggling with executive functioning at work, it's time to seek professional insight. A formal evaluation can provide a clear picture of your mental health. I believe that early intervention is key to preventing the symptoms from becoming a deeply ingrained part of your identity.
What happens if persistent depressive disorder is left untreated?
Leaving PDD untreated increases the risk of developing "double depression," where episodes of major depressive disorder are superimposed on the chronic low mood. Statistics indicate that up to 75% of individuals with untreated PDD will experience at least one major depressive episode. Chronic untreated depression also correlates with physical health issues, including a 40% higher risk of developing cardiovascular disease. Seeking a diagnosis helps us build a roadmap to prevent these more severe health complications.
