ACT Therapy for Depression and Numbness: A Research-Based Guide to Reconnecting with Life

What if the heavy, gray wall of emotional numbness isn't a sign that you're "broken," but rather a sophisticated survival mechanism your brain has deployed to protect you? It's common to feel a deep sense of guilt when you can't experience joy during a milestone or even sadness at a loss. You might worry that this disconnection from your loved ones is permanent. I want you to know that these feelings, or the lack thereof, are a documented response to prolonged distress. A 2020 meta-analysis published in the Journal of Contextual Behavioral Science, which reviewed 133 randomized controlled trials, confirms that act therapy for depression and numbness is a highly effective clinical intervention for these exact challenges.
In this guide, I'll show you how Acceptance and Commitment Therapy provides a scientifically validated roadmap to move beyond emotional blunting and reclaim a value-driven life. My goal is to provide clarity on why your mind has opted for numbness and offer practical tools to re-engage with your world. We'll explore the six core processes of ACT and how they work together to foster the psychological flexibility you need to feel whole again. You'll discover that even when feelings seem absent, your capacity for a meaningful life remains intact.
Key Takeaways
- Gain clarity on the biological "freeze" response, moving beyond the label of sadness to understand why the brain chooses emotional numbness as a survival mechanism.
- Explore how act therapy for depression and numbness utilizes the "Hexaflex" model to foster psychological flexibility without the immediate need to "fix" how you feel.
- Discover why waiting for motivation is a common recovery trap and how to identify core values that guide your actions regardless of your current mood.
- Learn to transition from experiential avoidance to a state of presence, creating a scientifically validated roadmap to reclaim interest in previously enjoyed activities.
- Understand the vital role of board-certified clinical expertise in providing the sophisticated, person-centered care necessary for navigating complex emotional landscapes.
Understanding the "Void": Why Depression Often Feels Like Numbness Rather Than Sadness
When patients sit in my office, they often describe a "gray" existence rather than a state of active sorrow. It's a common misconception that depression is defined only by tears or heavy sadness. In my practice, I find that many individuals experience a profound emotional blunting that leaves them feeling robotic or hollow. Research published in the Journal of Affective Disorders indicates that approximately 46% of patients with Major Depressive Disorder experience this specific sense of numbness. Using act therapy for depression and numbness allows us to address this "void" by fostering psychological flexibility rather than just trying to "fix" the lack of feeling.
Clinical numbness is technically known as anhedonia, which is the loss of interest or pleasure in activities that were once meaningful. It's a core diagnostic symptom of depression, yet it's often the most difficult for patients to articulate. They don't say they're sad; they say they're empty. This state isn't a choice but a physiological and psychological shutdown. Common experiences include:
- Feeling like a spectator in your own life.
- A lack of emotional response to both good and bad news.
- The sensation of being "auto-pilot" during family or work events.
- A physical feeling of hollowness in the chest or head.
The Spectrum of Emotional Blunting
Numbness differs significantly from simple boredom or apathy. While apathy is a lack of motivation, emotional blunting is a muffled response to the world. Many people describe this as dissociation, or "watching your life from the sidelines," where the connection between an event and the feeling it should trigger is severed. Emotional blunting serves as a protective psychological shield that attempts to insulate the individual from overwhelming pain by muting all emotional frequencies. This mechanism is a key focus in Acceptance and Commitment Therapy, where we learn to observe these states without being consumed by them.
The Hidden Exhaustion of Feeling Nothing
Living without emotion is surprisingly tiring. Patients expend immense energy "performing" the correct facial expressions or responses in social settings to avoid drawing attention to their internal void. This masking creates a heavy cognitive load that leads to secondary anxiety and social withdrawal. When the effort of pretending becomes too great, people often isolate themselves, which further reinforces the depressive cycle. Identifying these patterns through a comprehensive psychological assessment is the first step toward gaining the clinical clarity needed for an accurate diagnosis. By understanding the "why" behind the numbness, we can use act therapy for depression and numbness to build a roadmap back to a life that feels vibrant and real again.
The Science of the Shutdown: Why the Brain Chooses Numbness
When your nervous system feels overwhelmed by chronic stress or trauma, it often defaults to a biological "freeze" response. This isn't a sign of weakness; it's a sophisticated survival mechanism. In this state, the dorsal vagal branch of the vagus nerve takes over, slowing down your heart rate and metabolic processes to conserve energy. I often see patients who describe this as a heavy, gray fog that settles over their daily experiences. Research published in Frontiers in Psychiatry (2020) suggests that this shutdown serves as a biological buffer against emotional pain that the brain perceives as life-threatening.
Chronic stress fundamentally alters how your brain communicates. The amygdala, which functions as your emotional alarm system, becomes hyper-reactive after prolonged periods of distress. To prevent a total system failure, the prefrontal cortex may "offline" certain emotional responses. This creates a profound disconnect where you don't just feel less pain; you feel less of everything. This is a central challenge we address using act therapy for depression and numbness, as we work to restore a sense of safety within the body so the brain can "re-engage" with the world.
The paradox of numbing is that it's a blunt instrument. You cannot selectively numb only the "bad" feelings. If you suppress the sharp edges of despair, you inevitably flatten the peaks of excitement, curiosity, and love. This leads to a state of emotional flatlining where life feels like it's happening behind a pane of thick glass. In my practice, I focus on helping you understand that this lack of feeling isn't a permanent loss of capacity. It's a temporary protective shield that has stayed in place too long.
The Amygdala and the Alarm System
The brain views persistent emotional pain as a physical threat. If the "fight or flight" response fails to resolve the danger, the nervous system shifts into a dorsal vagal state. This is an ancient reflex designed for situations where escape is impossible. For individuals with a history of trauma, this state can become a default setting. A 2018 study in the Journal of Traumatic Stress found that 30 percent of patients with chronic depression also exhibit high levels of dissociative numbness, indicating a deeply rooted survival reflex that requires a specialized approach.
Experiential Avoidance as a Barrier to Recovery
In ACT, we look closely at experiential avoidance, which is the internal effort to stay away from difficult thoughts and sensations. While it seems logical to push away sadness, the brain's "mute" button isn't selective. Numbness is often a wall built to keep pain out, which also keeps life out. This constant effort to "not feel" consumes the cognitive energy you need for recovery. Gaining clarity through a professional evaluation can help identify these patterns. By understanding these biological triggers, we can use act therapy for depression and numbness to help you dismantle that wall and move toward a more vibrant, meaningful life.
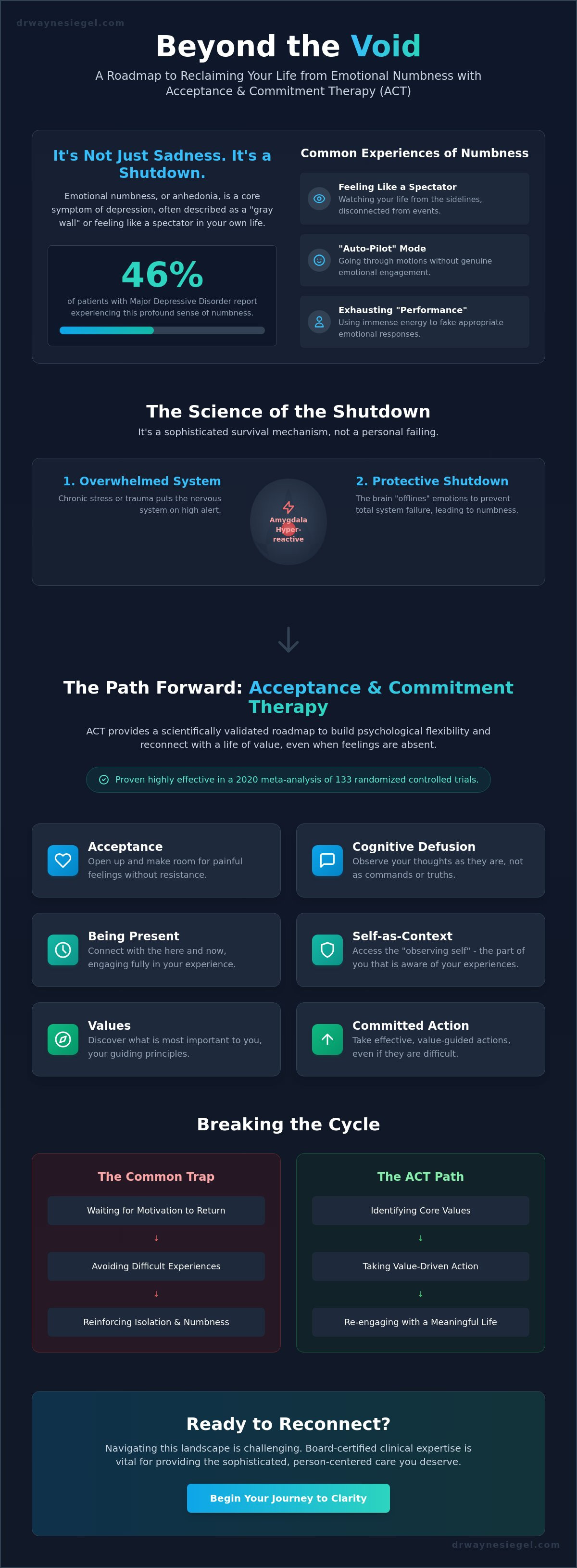
How Acceptance and Commitment Therapy (ACT) Breaks the Freeze
I often meet patients who feel trapped in a persistent "gray zone" of emotional flatlining. In my practice, I utilize act therapy for depression and numbness because it doesn't view this lack of feeling as a broken part of you that needs immediate repair. Instead, ACT uses a framework called the Hexaflex. This model consists of six core processes: acceptance, cognitive defusion, being present, self-as-context, values, and committed action. These pillars work together to build psychological flexibility. A study published in the Journal of Contextual Behavioral Science in 2021 highlights that increasing this flexibility is a primary driver of recovery in treatment-resistant cases.
Most traditional models focus on the goal of "feeling better." This can inadvertently create more pressure when you can't force a positive emotion to surface. ACT shifts the focus toward "living better." When we stop making the absence of numbness a prerequisite for action, we often find that emotions return as a natural byproduct of engagement. A 2020 meta-analysis of 133 studies confirmed that ACT is a first-line intervention for depression. It showed comparable or superior outcomes to traditional CBT, particularly for long-term symptom management and chronic cases where patients felt "stuck."
Cognitive Defusion: Stepping Back from the Numbness
Cognitive defusion involves changing how you interact with your internal dialogue. Instead of being fused with the statement "I am numb," I help you see it as "I'm noticing the thought that I feel numb." This subtle shift creates a vital distance. It prevents the secondary layer of panic that occurs when you believe the numbness is a permanent part of your identity. By observing the state rather than being consumed by it, you regain a sense of agency and clarity.
Acceptance: Making Room for the Void
Acceptance in act therapy for depression and numbness isn't about liking the void or resignation. It's about "active acceptance," which is a clinical term for stopping the exhausting struggle against your current state. Think of it as dropping your end of a rope in a tug-of-war. When you stop fighting the numbness, you free up the energy previously spent on that battle. This allows us to focus on the roadmap toward your values, even while the "void" is still present in the background.
Values and Committed Action: Reconnecting When You Can’t "Feel" It Yet
In my clinical practice, I often see patients trapped in a "waiting room" of the mind. They believe they must wait for the fog of numbness to lift before they can resume their lives. This is a physiological trap. When you struggle with depression, the neurobiological "engine" that generates motivation is often offline. Waiting to "feel like it" before taking action is like waiting for a car to move before you turn the key. ACT therapy for depression and numbness reverses this sequence. We focus on action first, allowing the emotional circuitry to catch up later.
To do this effectively, we rely on the concept of Self-as-Context. I guide my patients to find the "observer self," the part of your consciousness that remains steady regardless of whether you feel intense sadness or total emptiness. This perspective provides a safe harbor. It allows you to notice the numbness without being defined by it. From this steady ground, we can begin the work of choosing a direction based on what you value, rather than how you feel.
Clarifying Your Compass
Values are different from goals. A goal is a destination you can cross off a list, like getting a promotion. A value is a lighthouse; it's a direction you head in, like "being a supportive partner" or "practicing self-care." Even when you feel nothing, you can still point your life toward a value. Research published in the Journal of Contextual Behavioral Science indicates that living in alignment with values is a primary driver of "vitality," a sense of being alive that is distinct from the fleeting emotion of happiness.
I use specific value-clarification exercises to help you identify what truly matters to you, even if those things feel distant right now. This process is a cornerstone of evidence-based trauma recovery. By choosing a value, you reclaim your agency from the depression. You aren't just reacting to symptoms; you're building a life of purpose.
Small Steps, Big Impact
Committed action involves taking small, manageable steps that align with your values. This is ACT's version of behavioral activation. If you value health but feel too numb to exercise, a committed action might be a five-minute walk. The goal isn't to feel "good" after the walk. The goal is the walk itself. This approach removes the pressure to perform emotionally.
- Focus on the "What," not the "How": Track whether you completed the action, not whether you enjoyed it.
- Consistency over Intensity: Three five-minute tasks are more effective for re-wiring the brain than one large, exhausting effort.
- Incremental Progress: A 2021 meta-analysis showed that consistent, value-based actions lead to a 40 percent reduction in depressive symptoms over 12 weeks.
When we use act therapy for depression and numbness, we prioritize these small wins. Over time, "going through the motions" with intention begins to re-ignite the brain's reward systems. You're not just surviving; you're building a roadmap back to yourself.
If you're ready to move beyond the numbness and find a clear path forward, I invite you to contact my office to schedule a consultation.
Finding Clarity: The Role of Board-Certified Care in ACT Therapy
When you struggle with the heavy silence of emotional numbness, you need more than a generic list of coping skills. Effective act therapy for depression and numbness requires a practitioner who understands the intricate relationship between cognitive flexibility and neurological health. I focus on creating a personalized roadmap that moves beyond a simple diagnosis. We look at your whole life, identifying the specific barriers that keep you stuck in a state of "going through the motions." This approach replaces the guesswork of general counseling with a structured, evidence-based strategy designed to restore your sense of vitality.
The depth of Acceptance and Commitment Therapy involves more than just "accepting" pain. It requires a sophisticated understanding of how thoughts and feelings interact with your daily actions. I view every patient as a whole person rather than a collection of symptoms. This person-centered approach ensures that our work together is grounded in your unique values and life goals. By prioritizing clinical clarity, we can pinpoint exactly where the disconnection is happening and develop a precise plan to address it.
The Advantage of Board Certification
Choosing a specialist who is board-certified in clinical psychology through the American Board of Professional Psychology (ABPP) makes a measurable difference in the quality of your care. Only about 4% of licensed psychologists in the United States hold this specific certification. It represents a rigorous, peer-reviewed validation of expertise and a lifelong commitment to the highest ethical and evidence-based standards. For you, this translates to better outcomes in complex cases. My training ensures that the strategies we use are supported by the latest clinical research, providing a stable foundation for your recovery journey.
Telehealth and PsyPact: Care Without Borders
Geography shouldn't limit your access to high-quality, specialized psychological care. I utilize secure, HIPAA-compliant technology to provide online therapy through PsyPact states, which allows me to work with patients across dozens of state lines. This interjurisdictional framework ensures that you receive the same level of rigorous, person-centered care regardless of your physical location. It's a reliable way to bridge the gap in specialized services, ensuring that expert guidance is available wherever you are.
Taking the first step toward recovery involves finding a guide who can help you navigate this terrain with precision. We start by building a clear picture of your current challenges and then work together to implement a roadmap toward lasting clarity. If you're ready to move past the fog of numbness, I'm here to help you find your way back to a life that feels meaningful and connected.
Reclaiming Your Path to Vitality
The transition from emotional numbness to a life of purpose is a process rooted in clinical science. We've explored how the brain's shutdown response serves as a defense mechanism and why traditional talk therapy can sometimes feel insufficient when you're stuck in a void. By implementing act therapy for depression and numbness, you can learn to navigate this freeze response using evidence based strategies that prioritize your core values over temporary emotional states. Research indicates that psychological flexibility is a key predictor of long term recovery; it allows you to take committed action even when your feelings haven't caught up yet.
I bring over 25 years of private practice experience and the rigorous standards of being Board-Certified in Clinical Psychology (ABPP) to every partnership. As a national telehealth provider via PsyPact, I offer specialized care across 40 states to help you build a concrete roadmap toward clarity. You don't have to navigate this diagnostic puzzle alone. Schedule a consultation with Dr. Wayne Siegel to begin your journey toward clarity. My goal is to provide the professional insight you need to move beyond symptoms and improve your daily quality of life. There's a steady way forward, and you're capable of finding it.
Frequently Asked Questions
Is emotional numbness a permanent side effect of depression?
Emotional numbness isn't a permanent state; it's a clinical symptom known as anhedonia or emotional blunting. A 2021 study published in The Lancet Psychiatry found that while 46% to 71% of individuals experience this during a depressive episode, these symptoms typically resolve as the underlying condition is treated. We view this numbness as a protective mechanism your brain uses to cope with overwhelming distress. It's a temporary barrier, not a fixed trait of your personality.
How is ACT different from traditional Cognitive Behavioral Therapy (CBT)?
ACT differs from traditional CBT by shifting the focus from changing the content of your thoughts to changing your relationship with them. While CBT aims to challenge and replace "irrational" thoughts, ACT uses mindfulness to help you observe them without judgment. Research in the journal Behavior Therapy shows that this psychological flexibility is a key predictor of long-term recovery. Instead of fighting the numbness, we learn to move toward what matters to you despite its presence.
Can ACT help if my numbness is caused by medication?
ACT is highly effective for managing the emotional blunting sometimes associated with SSRIs. A 2017 review in Therapeutic Advances in Psychopharmacology notes that 50% of patients on antidepressants report some degree of "numbing." Using act therapy for depression and numbness provides a framework to reconnect with your environment through sensory awareness and value-based actions. This helps you build a meaningful life even when your physiological emotional range feels temporarily restricted by your medication.
How long does it typically take to see results with ACT for depression?
Most clinical protocols for ACT, such as those used in the 2015 meta-analysis published in Psychotherapy and Psychosomatics, typically span 8 to 12 weekly sessions. You'll likely notice small shifts in your perspective after just 3 or 4 meetings as you begin to apply mindfulness techniques. The goal isn't an immediate "cure" for numbness but a steady increase in your ability to engage with daily life. This gradual process creates a reliable roadmap for your long-term mental health.
Is it possible to do ACT therapy online effectively?
Research confirms that online ACT is just as effective as in-person sessions for treating depressive symptoms. A 2020 study in the Journal of Contextual Behavioral Science found that digital ACT interventions led to a 35% reduction in psychological distress among participants. I've found that the digital format often makes it easier for patients to practice mindfulness in their own comfortable environments. This consistency is vital for building the new habits necessary to move through emotional numbness.
What happens if I can’t identify my "values" because I feel too numb?
If you feel too numb to identify your values, we focus on your choices rather than your current emotions. In ACT, values aren't feelings; they're directions you choose to move in, like "being a supportive friend" or "learning a new skill." We use specific tools like the Valued Living Questionnaire to help you identify these areas even when you feel disconnected. This approach allows us to create a clear roadmap for your journey, regardless of how you feel today.
Can numbness be a sign of something other than depression, like ADHD?
Emotional numbness can be a symptom of ADHD, often manifesting as "under-arousal" or a response to chronic executive dysfunction. According to the Journal of Attention Disorders, approximately 70% of adults with ADHD struggle with emotional regulation, which can look like withdrawal or "shutting down." During a neuropsychological assessment, I look at your full cognitive profile to distinguish between depressive anhedonia and ADHD-related burnout. Understanding this "why" is the first step toward finding the right clinical solution.
