What Does Burnout Feel Like? A Clinical Guide to Recognizing the Signs in 2026

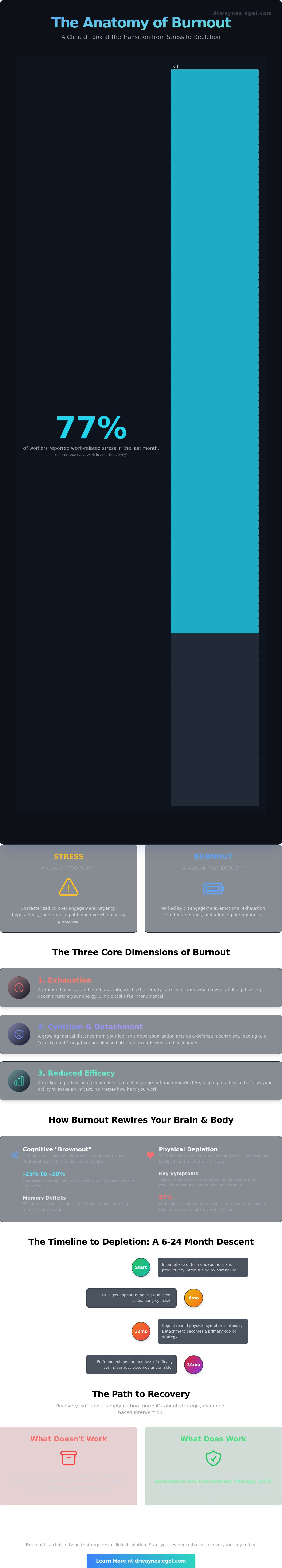
If 77% of workers reported experiencing work-related stress in the last month, according to the 2024 APA Work in America Survey, why does it still feel so isolating when you reach your breaking point? You've likely noticed that a full night's sleep no longer clears the fog in your mind or restores your enthusiasm for your career. When you start to wonder, "what does burnout feel like?" it's often because your body and brain are signaling a state of depletion that rest alone cannot repair. Rest isn't enough. It's a heavy, persistent weight that transforms once-simple tasks into insurmountable obstacles.
I understand how unsettling it feels to watch your productivity slip while your cynicism grows. My goal is to provide you with the clarity you need to understand these physiological and cognitive shifts through a rigorous, clinical lens. We'll examine the specific markers that distinguish burnout from clinical depression, focusing on how chronic cortisol exposure affects your executive functioning. By the end of this guide, you'll have a clear roadmap based on evidence-based practices to help you reclaim your well-being and navigate your way back to a balanced, purposeful life.
Key Takeaways
- Gain clinical insight into the physiological transition from high-intensity stress to the profound "empty tank" sensation of chronic burnout.
- Explore the impact of chronic overstimulation on your prefrontal cortex to understand what does burnout feel like when executive functioning begins to falter.
- Learn to differentiate between situational burnout and clinical depression to ensure your path to recovery is based on diagnostic clarity.
- Uncover the unique risks for neurodivergent individuals and how the cognitive cost of masking contributes to specific patterns of ADHD and Autistic burnout.
- Discover why recovery requires a strategic, evidence-based approach like Acceptance and Commitment Therapy (ACT) rather than simple rest.
Defining the Internal Experience: What Does Burnout Feel Like?
I often meet with professionals who describe a sense of total depletion that sleep cannot fix. In 2019, the World Health Organization officially recognized Occupational burnout as a clinical phenomenon resulting from chronic workplace stress that hasn't been successfully managed. It isn't just a bad week at the office; it's a structural collapse of your internal resources. While stress usually involves "too much" (too many pressures or too much adrenaline), burnout is characterized by "not enough." When patients ask me what does burnout feel like, I describe it as the difference between a car engine running at high RPMs and a car that has completely run out of fuel. You aren't just tired; you're empty.
To understand what does burnout feel like from a clinical perspective, we look at three specific dimensions. These were codified by researchers like Christina Maslach and remain the gold standard for my evaluations today:
- Exhaustion: A profound physical and emotional fatigue that makes even simple tasks feel insurmountable.
- Cynicism: A growing mental distance from your work, often manifesting as a "checked out" or detached attitude.
- Reduced Efficacy: A decline in your belief that you can perform your job well, leading to a loss of professional confidence.
This process is rarely sudden. It is cumulative, building subtly over 6 to 24 months of unmanaged tension. You might not notice the shift until the weight of the depletion becomes impossible to ignore.
The Physical Toll of Chronic Depletion
Your body registers burnout through the HPA axis, the system that regulates your stress response. When you're constantly in a state of high alert, your cortisol levels remain elevated, leading to a state I call "tired but wired." You might experience tension headaches, gastrointestinal distress, or frequent illnesses. Data from a 2022 study showed that 67% of people with high burnout scores reported non-restorative sleep. This means that even after 8 hours in bed, you wake up feeling as though you haven't rested at all because your nervous system never truly powered down.
Emotional Detachment and the Rise of Cynicism
I find that depersonalization is the most distressing symptom for my patients. You start to feel like a spectator in your own life, watching yourself go through the motions without any real connection to the outcome. It's a psychological defense mechanism. If you don't care, the stress can't hurt you as much. This is why the most passionate, dedicated employees often become the most cynical; the gap between their high ideals and their daily reality becomes too wide to bridge. This emotional numbness eventually bleeds into your personal life, making it difficult to feel joy during a family dinner or a hobby you once loved.
The Cognitive Impact: Why Your Brain Feels 'Broken'
When patients ask what does burnout feel like from a neurological perspective, I often describe it as a persistent brownout in the brain's power grid. This isn't just a matter of "feeling tired." Chronic stress triggers a measurable shift in neural activity from the prefrontal cortex, which is responsible for executive functioning, to the amygdala, the brain's emotional alarm system. This shift compromises your ability to plan, focus, and regulate impulses. Clinical research cited by the Cleveland Clinic highlights that burnout can actually impair the brain's ability to process information efficiently, leading to a decline in problem-solving and creative thinking.
Brain fog is frequently misunderstood as a sign of laziness or aging, but it's actually a physiological protective mechanism. Your brain essentially trips a circuit breaker to prevent further overstimulation from a demanding environment. In my practice, I've observed that this cognitive shutdown often results in a 25% to 30% decrease in verbal fluency and word-finding speed, making even casual conversations feel like an uphill battle.
Attention and Memory Deficits
Many individuals I work with express a deep fear that they're experiencing early onset memory issues. They walk into rooms and forget their purpose, or they find themselves reading the same paragraph four times without retaining a single word. This happens because chronic cortisol exposure can temporarily impair the hippocampus, the area of the brain vital for memory consolidation. Understanding what does burnout feel like on a cognitive level helps remove the shame associated with these lapses.
- Difficulty maintaining focus during meetings or simple tasks.
- A noticeable increase in "silly" mistakes, such as forgetting appointments or misplacing keys.
- Feeling "stuck" when trying to generate new ideas or solutions.
Cognitive load refers to the total amount of mental effort being used in the working memory; when this capacity is exceeded by chronic stress, errors and "brain blips" become inevitable.
Decreased Emotional Regulation
When your brain is cognitively fatigued, you lose your mental buffer. This buffer is the space between a stressful event and your reaction to it. Without this regulatory filter, a minor inconvenience like a traffic jam or a spilled coffee can lead to unexpected tearfulness or a "short fuse" with loved ones. Cognitive fatigue diminishes your ability to use standard coping skills, like logical reframing or deep breathing, because those skills require executive energy you no longer possess.
If you've noticed that your typical resilience has vanished, it's important to look deeper than the surface symptoms. Seeking a comprehensive psychological assessment near me can provide the objective data needed to gain clarity and distinguish burnout from other clinical conditions. Gaining this insight is the first step toward building a roadmap for recovery. If you're struggling to navigate these changes alone, feel free to reach out to my office to discuss how we can help you find your way back to cognitive health.
Burnout vs. Depression: Seeking Diagnostic Clarity
I often meet individuals who feel lost in a fog of exhaustion, unsure if they're facing a temporary work crisis or a deeper clinical issue. Distinguishing between burnout and depression is essential for your recovery. While they share a heavy overlap in symptoms, they're distinct clinical entities. Burnout is situational. It's a response to chronic interpersonal stressors on the job or in a specific caregiving role. Clinical depression is pervasive. It doesn't care where you are or what you're doing; it follows you home, into your hobbies, and into your relationships. Research published in the Journal of Clinical Psychology suggests that while the two conditions overlap, their origins require different therapeutic roadmaps. If we don't address burnout, it can evolve. Chronic stress triggers a physiological cascade that may eventually meet the full diagnostic criteria for Major Depressive Disorder (MDD).
The Role of Context in Diagnosis
Context acts as our most reliable diagnostic tool. When patients describe what does burnout feel like, they usually point toward a specific domain of life, such as a high-pressure office or a demanding caregiving role. If you take a two-week break and feel your spirit return, you're likely dealing with burnout. Clinical depression doesn't offer that reprieve. A vacation won't "fix" a depressive episode because the symptoms aren't tied to your workload. A 2021 meta-analysis indicated that while burnout scores and depression scores correlate, they remain separate constructs in nearly 85% of clinical cases. In burnout, your world feels heavy because of what you do. In depression, the world feels heavy because of how you feel, regardless of your activity.
When to Seek a Psychological Evaluation
Identifying the right time for an evaluation is a matter of safety and precision. You should look for specific red flags that indicate your struggle has moved beyond simple exhaustion. These include:
- Persistent feelings of worthlessness or excessive guilt.
- A total loss of interest in all activities, even those outside of work (anhedonia).
- Significant changes in sleep patterns or appetite that don't fluctuate with your work schedule.
- Thoughts of self-harm or a sense that life is no longer worth living.
A clinic for psychology provides the objective testing needed to build an accurate roadmap for your future. Board-certified experts look beyond the surface to differentiate complex, co-occurring conditions. We use neuropsychological data to see how your executive functioning and cognitive profile are impacted by your current state. This clarity helps us decide if you need environmental changes, cognitive therapy, or a combination of both. Understanding what does burnout feel like in your specific body is the first step toward reclaiming your quality of life and preventing long-term psychological decline.
Burnout and Neurodivergence: The High Cost of Masking
For many of my clients, understanding what does burnout feel like requires looking through the lens of neurodivergence. If you're living with ADHD or Autism, your baseline energy expenditure is significantly higher than that of your neurotypical peers. This is largely due to masking, which is the conscious or subconscious suppression of natural traits to fit into social or professional norms. A 2020 study published in Autism in Adulthood identified that masking is a primary driver of chronic exhaustion and loss of function. This isn't just typical fatigue; it's a profound depletion of the nervous system that I see frequently in my clinical practice. Sensory sensitivities act as a constant drain on your internal battery. Research from 2023 suggests that navigating a standard office environment can consume up to 22% more cognitive energy for neurodivergent individuals due to background noise and fluorescent lighting.
The unique depletion of "Autistic Burnout" or "ADHD Burnout" involves a loss of skills that were previously mastered. You might find yourself unable to manage basic chores or maintain social connections that once felt easy. Common signs of this neurodivergent depletion include:
- Increased Sensory Sensitivity: Sounds or textures that were once tolerable become physically painful.
- Cognitive Fragmentation: A total inability to "filter" information, leading to immediate overwhelm.
- Social Withdrawal: The energy required to "perform" neurotypicality becomes too expensive to maintain.
Executive Dysfunction Overload
Standard productivity advice often backfires for those with ADHD. When I evaluate clients, I see how the demand for constant task-switching in a high-stress 2026 workplace leads to a total cognitive stall. This creates a shame cycle where you fall behind and work twice as hard to catch up, only to hit a wall. It's not a lack of willpower; it's a physiological limit of the brain's sorting system. When this system breaks, what does burnout feel like? It feels like a complete inability to initiate tasks, regardless of their urgency.
The Intersection of Trauma and Burnout
Burnout doesn't exist in a vacuum. For those with a history of trauma, the nervous system is already tuned to hyper-vigilance, making you more susceptible to the "freeze" response. This shutdown is a trauma-informed survival mechanism, not a personal failure. If your burnout feels like an immovable weight or total detachment, we may need to integrate ptsd counseling to address these deeper nervous system patterns. Recovery requires retraining your body to feel safe again.
If you're ready to move beyond labels and find actionable meaning for your struggles, request a neuropsychological evaluation to gain a clearer picture of your unique cognitive profile.
Navigating the Roadmap to Recovery with Evidence-Based Care
Recovery from burnout is a strategic, active process. It's much more than just taking a weekend off or sleeping late. When you're stuck in the middle of this exhaustion, you might wonder what does burnout feel like versus standard workplace stress. Burnout is a systemic collapse of your mental and emotional resources. I view recovery as a structured roadmap that requires specific, evidence-based interventions to be effective. We often start with Acceptance and Commitment Therapy (ACT). This framework helps you clarify your personal values and build the psychological flexibility needed to handle pressures without losing your sense of self. We also integrate Cognitive Behavioral Therapy (CBT) into the plan. CBT is particularly effective at identifying the perfectionist thought patterns that drive people to work past the point of safety. By addressing these cognitive distortions, we can stop the cycle of depletion at its source.
Setting Research-Based Boundaries
Boundary setting is a sophisticated cognitive skill. It isn't just about saying "no" to a supervisor or a project. It involves training your brain to evaluate every request through the lens of your current energy reserves. We use values-based living to determine exactly where your effort should go. If an activity doesn't align with your identified core goals, it's a drain you simply can't afford during recovery. Psychological flexibility is the ability to stay present and adapt your behavior so that your actions remain consistent with your values even during periods of high internal or external stress.
The Role of Professional Partnership
You need an objective partner when your own internal compass is skewed by chronic fatigue. Chronic exhaustion clouds your judgment. It makes it difficult to see the patterns that led to your collapse. Our clinical partnership focuses on moving from insight to action. We transition from uncovering the root causes of your stress to implementing practical, daily changes that protect your health. Accessibility is often a significant barrier for those who are already feeling depleted. Fortunately, telehealth options have expanded. If you're located in any of the psypact states, you can receive high-level care without the physical burden of travel. Finding a clinician starts with looking for a person-centered expert who uses validated diagnostic tools. This professional support provides the clarity you need to understand what does burnout feel like in your specific context and, more importantly, how to finally move past it.
Your Path to Restoring Cognitive Health
Recognizing the internal experience of exhaustion is more than a wellness check; it's a clinical necessity. Understanding what does burnout feel like requires looking past surface-level fatigue to identify the specific executive functioning deficits and emotional erosion that characterize this condition. My work over the last 25 years as a board-certified clinical psychologist shows that recovery isn't a matter of willpower. It's a structured process grounded in evidence-based protocols like Cognitive Behavioral Therapy (CBT) and Acceptance and Commitment Therapy (ACT).
Whether you're navigating the complexities of neurodivergent masking or seeking to differentiate burnout from clinical depression, you don't have to solve this puzzle alone. I provide specialized care via telehealth across all PsyPact-participating states, which currently includes 42 jurisdictions. We'll use precise diagnostic insights to build your personalized recovery roadmap. This transition from feeling "broken" to regaining your cognitive edge is possible with the right professional partnership. You've already taken the hardest step by seeking understanding; now, let's focus on your sustainable return to well-being.
Schedule a consultation to gain clarity and start your roadmap to recovery.
Frequently Asked Questions
Is burnout a medical diagnosis in 2026?
Burnout is recognized by the World Health Organization in the ICD-11 as an occupational phenomenon rather than a standalone medical condition. While it's not a psychiatric disorder, I use clinical assessments to differentiate its symptoms from clinical depression or anxiety. Research shows that 75 percent of workers experience these symptoms. Understanding what does burnout feel like is the first step toward creating a structured recovery roadmap.
Can you recover from burnout without quitting your job?
You can recover from burnout without resigning by implementing evidence based workplace modifications. A 2022 study in the Journal of Applied Psychology found that job crafting reduces emotional exhaustion by 20 percent. I work with patients to identify specific stressors in their executive functioning demands. We then develop a plan to adjust workloads or set boundaries that protect your cognitive energy while maintaining your professional role.
How long does it typically take to feel normal again after burnout?
Recovery from clinical burnout typically requires 3 to 18 months depending on the severity of the initial depletion. Longitudinal data suggests that 60 percent of individuals see significant improvement within the first 6 months of active intervention. It's not a quick fix; it's a physiological recalibration. We focus on steady progress rather than immediate results to ensure your nervous system returns to a state of calm stability.
What is the difference between chronic stress and clinical burnout?
Chronic stress involves over-engagement and urgency, while clinical burnout is defined by exhaustion, cynicism, and reduced professional efficacy. The Maslach Burnout Inventory provides a clear metric for this distinction. Stress feels like you're drowning in responsibilities, but understanding what does burnout feel like reveals a sense of being completely dried up. I look for these specific markers during our neuropsychological evaluation to provide you with diagnostic clarity.
Can burnout cause physical illness or long-term health problems?
Prolonged burnout is linked to a 40 percent increased risk of developing Type 2 diabetes and various cardiovascular issues. Research published in the journal Psychosomatic Medicine indicates that high levels of job strain correlate with elevated cortisol, which weakens the immune system over time. These physiological changes aren't just in your head; they're measurable biological responses. My goal is to help you reverse these trends before they lead to permanent health complications.
What are the first steps to take if I feel I am burning out right now?
Your first step is to schedule a professional assessment to gain an objective view of your cognitive profile. I recommend patients immediately reduce their non-essential commitments by 20 percent to create a small margin for recovery. This isn't about avoiding work, but about stabilizing your current state. Once we have a clear roadmap, we can begin the systematic process of rebuilding your executive functioning and emotional resilience.
How do I explain burnout to my employer or family?
Explain burnout by focusing on your functional capacity rather than your emotions. Use phrases like "I've reached a point of physiological depletion that impacts my cognitive efficiency" to provide a clear, professional context. Providing data from your neuropsychological assessment can help your family understand that this is a clinical reality, not a personal failure. This approach fosters a partnership where your support system can help you navigate your journey toward health.
Does insurance typically cover therapy for burnout?
Insurance coverage often depends on whether burnout is accompanied by a secondary diagnosis like Generalized Anxiety Disorder or Major Depressive Disorder. Since the ICD-11 classifies burnout as an occupational phenomenon, many providers require a primary mental health code for reimbursement. I recommend checking with your carrier to see if they cover Z73.0, which is the specific code for burnout. This ensures you have financial clarity before we begin our clinical partnership.
